Ulcerative colitis
The diagnosis for a chronic disease, such as ulcerative colitis, can cause concern about the effects it can have on a patient’s health and lifestyle.
However, modern Medicine and Surgery can offer solutions for effective disease management, allowing patients to live a healthy and normal life.
Dr. Konstantinidis and his Surgical Team specialize in the surgical treatment of ulcerative colitis with minimally invasive techniques, such as laparoscopy and -mostly- robotic surgery.
The use of the state-of-the-art robotic system, da Vinci Xi, at Athens Medical Center, ensures an optimal medical outcome with the least possible risk of injury to the patient’s tissues and consequent complications.
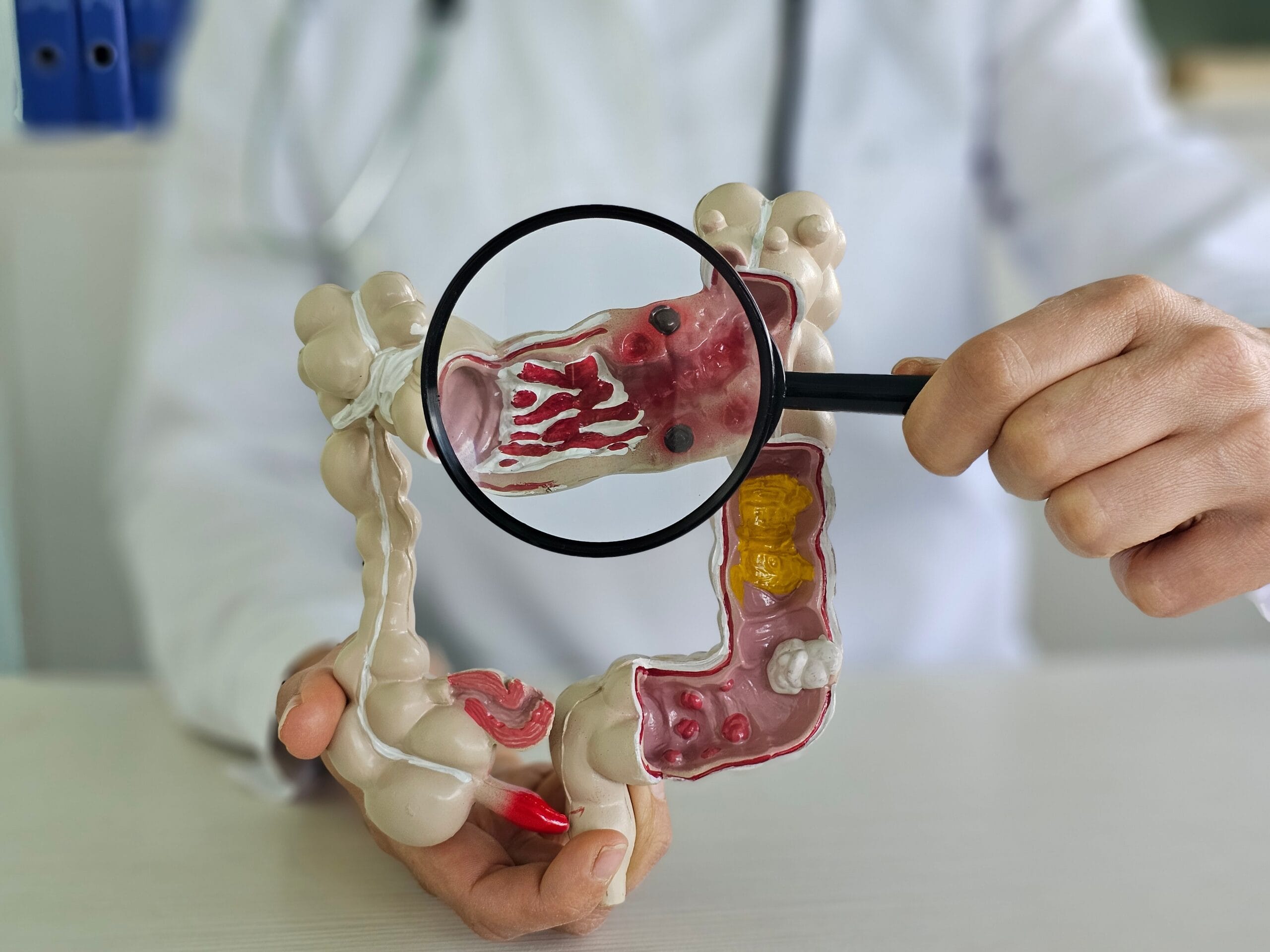
What is Ulcerative Colitis?
Ulcerative colitis is an idiopathic inflammatory disease characterized by inflammation of the lining of the colon and rectum.
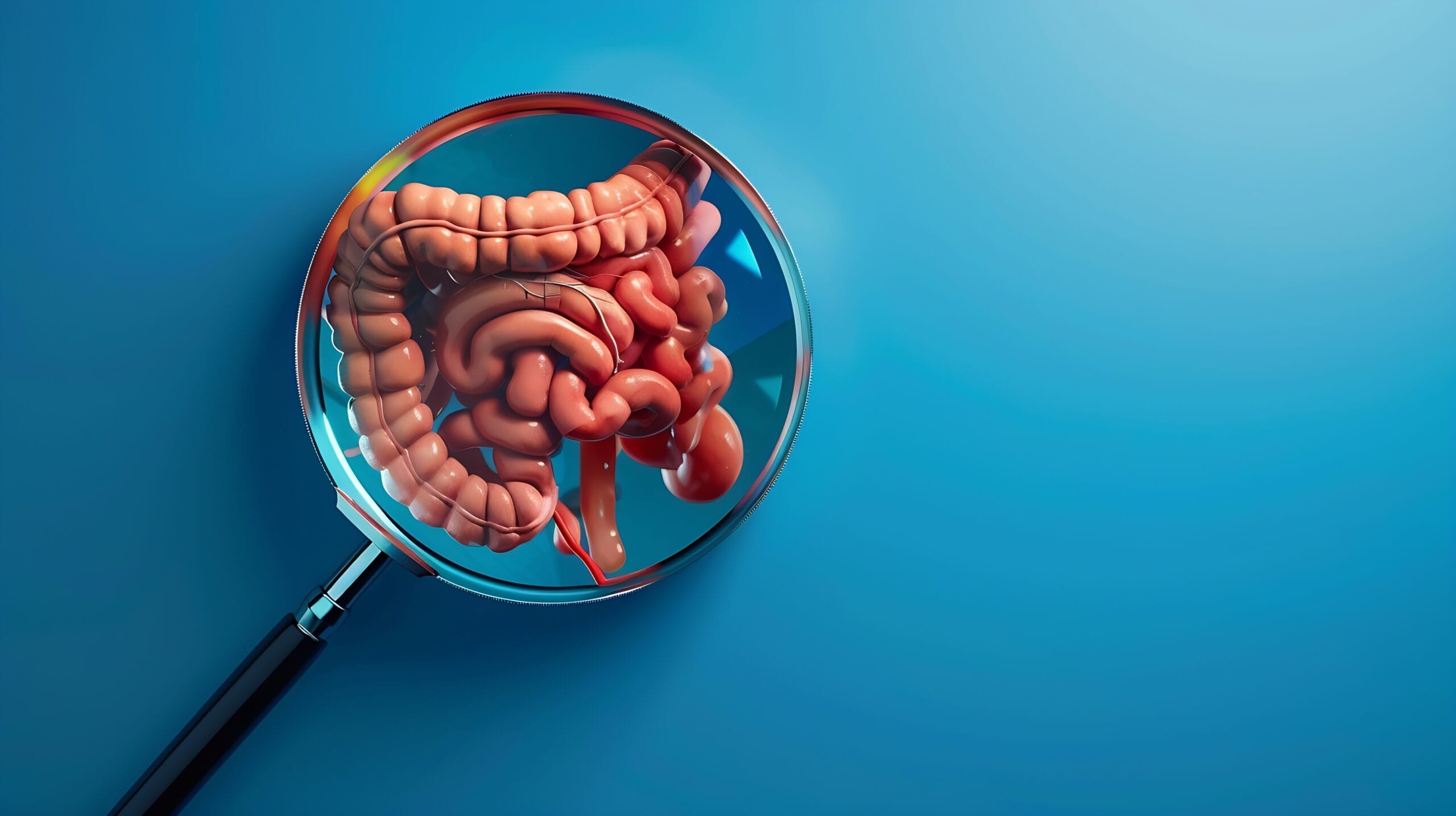
Although ulcerative colitis usually affects the lower part of the large intestine (the rectum), in some patients it may extend to the entire colon.
Ulcerative colitis belongs to a group of diseases called inflammatory bowel diseases, which also includes Crohn’s disease.
Why choose Dr. Konstantinidis?
Dr. K. M. Konstantinidis and his team possess vast experience in the field of laparoscopic and robotic surgery.
Dr. Konstantinidis is the pioneer of Robotic Surgery in Greece and one of the leading figures internationally in the field, having performed the largest series of General Surgery operations in Europe with the innovative Da Vinci® robotic system, including inguinal hernia surgeries.
What are the symptoms of Ulcerative Colitis?
The symptoms of ulcerative colitis depend on the severity of the inflammation and the length of the colon affected by the disease.
In patients with mild to moderate inflammation, symptoms may include:
rectal bleeding
diarrhea
mild abdominal cramps
incontinence
discomfort and feeling that you have not completely emptied the rectum after a bowel movement
When there is more severe inflammation, patients often experience:
fever
dehydration
severe abdominal pain
weight loss and appetite
developmental delay (in children and adolescents)
What are the causes of Ulcerative Colitis?
The causes of ulcerative colitis are still poorly understood.
According to the prevailing theories, the causes may include a combination of:
- the unique genetic composition of an individual
- environmental factors and
- specific characteristics of the patient’s immune system
How Is Ulcerative Colitis related to colon cancer?
Ulcerative colitis is known to increase the risk of colon cancer. People who have had ulcerative colitis for a long time are at a higher risk of developing colon cancer.
Statistics show that the chance of developing colon cancer begins to increase a few years after the onset of ulcerative colitis symptoms.
Colon cancer is a rare complication and is believed to be preventable by screening for inflammation of the colon as well as regular colonoscopy, which detects any pre-cancerous lesions in a timely manner.
How is Ulcerative Colitis diagnosed?
Ulcerative colitis is diagnosed based on the symptoms during a physical examination by a doctor, but confirmation of the diagnosis requires a series of tests, such as:
- Blood test. It is often performed to look for signs of inflammation or anemia (low redness), although these tests may be normal in patients with a mild illness.
- Fecal test. Its purpose is to look for signs of intestinal infection.
- Endoscopic examination. Colonoscopy or flexible sigmoidoscopy is usually performed in patients with symptoms to confirm the diagnosis.

Colectomy
How is Ulcerative Colitis treated?
The treatment of ulcerative colitis generally focuses on two separate goals:
- causing the disease to subside and
- preventing relapse
Depending on the case, treatment can be conservative, with the use of medication.
However, if the disease and consequent damage to the large intestine is extensive and if patients do not respond to medication or are worried or have unacceptable side effects from medication, then ulcerative colitis is treated surgically.
The most common surgery is colectomy.
There are two types of colectomy depending on whether the entire colon and rectum are removed or part of them:
- Total colectomy: In total colectomy, the entire large intestine and rectum are removed (proctocolectomy) and an Ileal Pouch Anal Anastomosis is performed, i.e. the small intestine is joined to the anus. In some, now rare, cases a permanent final ileostomy is performed (a temporary or permanent opening, called a stoma, that allows solid waste and gas exit the body without passing through the colon or the rectum).
- Partial colectomy: In partial colectomy, only the part of the intestine where the problem is located is removed. Depending on the part of the intestine that is removed, there are segmental, left or right colectomy and sigmoidectomy.
Colectomy can be performed with open surgery, laparoscopy or robotic surgery.
The conventional “open” colectomies are particularly traumatic procedures, because the surgeon is forced to make a large incision in the abdomen.
Thus, the injury from the surgery is significant and patients often face a long and difficult recovery period.
That is why in recent years it has become common in specialized centers for colectomies to be performed with minimally invasive methods, such as laparoscopy and evolution, robotic surgery.
Laparoscopic Colectomy
What is Laparoscopic Colectomy?
In laparoscopic colectomy, the surgeon makes 4 or 5 small incisions from which the specialized laparoscopic surgical instruments are inserted, such as the laparoscope, a tiny telescope connected to a video camera, that allows the surgeon to view the patient’s internal organs magnified on a monitor.
The damaged part of the intestine is then removed through one of the small incisions that is slightly widened for that purpose.
What are the advantages of Laparoscopic Colectomy?
Laparoscopic colectomy is characterized by all the advantages of minimally invasive techniques, such as:
- minor surgical injury
- minimal blood loss
- faster bowel function
- less postoperative pain
- optimal cosmetic outcome
- shorter hospital stay
- faster return to a solid food diet and to daily activities
Robotic Colectomy
What is Robotic Colectomy?
Robotic colectomy is the evolution of laparoscopic colectomy involving of a robotic system, which consists of an advanced surgical robot (da Vinci Xi) and a console, in which the surgeon is seated.
Navigating the robotic arms from the console, the surgeon makes 5-7mm micro-incisions, as performed in laparoscopy. However, in robotic colectomy the surgical field is now fixed and three-dimensional and the surgeon has a huge degree of freedom in the movement of surgical instruments.
Robotic surgical instruments are smaller and allow easier access to anatomically difficult areas.
In addition, with robotic colectomy, intra-abdominal anastomoses (re-uniting the intestine after removal of the affected part) is performed with greater comfort and safety than in laparoscopy.
What are the advantages of Robotic Colectomy?
Robotic colectomy incorporates all the advantages of laparoscopic colectomy offering additional capabilities to the surgeon.
The surgeon is seated on a special console, without getting tired, from which he navigates the special, robotic arms that perform the operation.
The arms have incomparable precision, flexibility and stability in their movements, while at the same time they allow access to even the most inaccessible parts of the abdomen.
Also, the three-dimensional display of the surgical field with great magnification on the console screen helps the surgeon feel as if he is inside the patient’s body!
Thus, the risk of injury to healthy tissues and organs during the operation is minimized, contributing to the faster healing and recovery of the patient.
Due to its ease of movement and 3D imaging, the da Vinci Xi HD robotic system is particularly useful and effective in certain phases of a colectomy (bowel mobilization, vascular control, maneuvers within a narrow pelvis, intra-abdominal suturing of anastomoses and nerve recognition).
When is Colectomy NOT recommended?
In a very small number of patients a laparoscopic / robotic colectomy may not be performed.
Factors that can increase the chances of having open surgery are:
- obesity
- a history of previous multiple abdominal surgeries, which may have caused many adhesions,
- hemorrhaging problems during the operation and
- the inability to get a clear image of the instruments
What is the postoperative course?
After the laparoscopic / robotic colectomy, patients get up on their feet and walk the very next day. This reduces muscle pain and significantly helps respiratory function.
On the third postoperative day patients are fed and discharged from the hospital very soon. They are deemed ready to return to their daily activities in about ten days.