Abdominal wall hernias
Hernias are an increasingly common cause for surgery, as a result of the increased incidence of obesity and chronic constipation associated with the contemporary, occidental lifestyle.
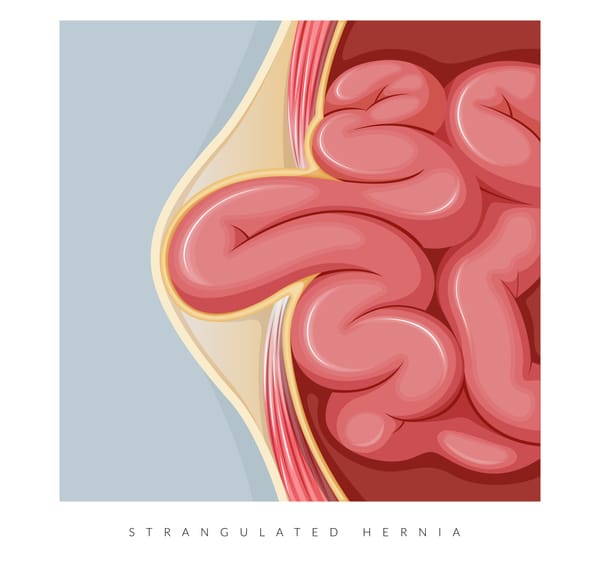
It is important that hernias are treated in a timely manner to avoid serious complications, such as strangulation that can cause intestinal obstruction and ischemia.
The only way for permanent correction of hernias is surgical repair, especially with the use of minimally invasive techniques, such as laparoscopy (performed through very small holes in the body) and its evolution, robotic hernia repair.
These minimally invasive techniques minimize the risk of complications and relapses, as well as the postoperative pain that follows conventional open surgery.
Dr. Konstantinidis and his Surgical Team have carried out a large number of hernia repair procedures, both laparoscopically and using the state-of-the-art robotic system, da Vinci Xi, at Athens Medical Center.

What is a Hernia?
A hernia is defined as a weak spot or an opening in the abdominal wall through which a viscera, such as the intestine, can pass through.
Many hernias occur in the abdomen (abdominal or epigastric hernias) but can also occur in the upper thigh (femoral hernias) and in the groin (inguinal hernias).
Most hernias are not immediately life threatening, but they do not go away on their own.
Sometimes they may require surgery to prevent dangerous complications.
A hernia can be congenital (i.e. since birth) or acquired (owing to tissue weakness or as a result of injury or surgery).
Hernias are quite common, affecting 10-15% of the population.
Both men and women can suffer from hernias.
Why choose Dr. Konstantinidis?
Dr. K. M. Konstantinidis and his team possess vast experience in the field of laparoscopic and robotic surgery.
Dr. Konstantinidis is the pioneer of Robotic Surgery in Greece and one of the leading figures internationally in the field, having performed the largest series of General Surgery operations in Europe with the innovative Da Vinci® robotic system, including inguinal hernia surgeries.
How can you tell if you have a Hernia?
Hernias are usually associated with a visible swelling or a bulge that results from the projection of an intra-abdominal viscera (most often intestine or fat) through an opening in the abdominal wall resulting in deformation of the skin surface.
Hernias can be manifested through discomfort or pain that is often associated with exercise. However, they may have no symptoms at all.
In the worst cases, hernias can cause severe pain or even blockage of the bowel (strangulated hernia).
If that happens patients must undergo surgery -at most- within six hours of the onset of symptoms, otherwise there is a risk of intestinal necrosis!!!
What are the symptoms of a Hernia?
Sometimes, hernias have no symptoms and can be detected unexpectedly as part of an examination for an unrelated problem.
However, quite often hernias are accompanied by characteristic symptoms, such as:
Swelling under the skin
Pain associated with exercise or weightlifting
Discomfort or pain especially when walking or running
Warning signs for hernia strangulation
Over time, hernias generally tend to grow, and their symptoms may deteriorate.
If neglected, a hernia can worsen to such an extent that it causes a strangulation, an emergency medical condition, which requires immediate surgery, to avoid serious complications that even reach the necrosis of the intestine!
The following signs are associated with the possibility of a strangulated hernia:
- Severe abdominal pain or abdominal distention (meteorism)
- Nausea and vomiting
- Redness, tenderness, or pain at the site of projection / swelling of the hernia
The only treatment for hernia is surgery.
How are Hernias caused?
Hernias are caused as a result of a combination of muscle weakness and stress.
Depending on the cause, a hernia can develop rapidly or over time.
Some common causes of muscle weakness or strain that can lead to a hernia include:
- previous surgeries and surgical incisions, which often weaken the abdominal wall and result in a hernia
- sudden increase in body weight
- chronic increase in intra-abdominal pressure
- lifting weights
- intense cough
- constipation
- dysuria (due to increased prostate gland size in men)
What are the risk factors for Hernia development?
There are a few factors that can increase the risk of developing a hernia, such as:
personal or family history of hernia
- age
- pregnancy
- obesity
- chronic constipation
- chronic cough
- cystic fibrosis
- smoking
- premature birth or low birth weight
Why do Hernias need to be treated?
The only way for permanent treatment of a hernia is surgical repair.
Patients with hernias are at risk of developing serious complications, such as the entrapment of the bowel in the hernia sac (strangulation) which can cause intestinal obstruction and ischemia (bowel perforation disorder leading to gangrene).
Both conditions require urgent surgical treatment.
Scheduled (non-emergency) hernia repair generally leads to better results, shorter recovery time, and far fewer postoperative complications.
What are the most common types of Hernia?
Hernias are classified based on the area they occur. The most common hernias develop in the groin. The main types of hernia that occur in this area of the body are inguinal hernia (direct or indirect) and femoral hernia.
In particular, hernias are divided into the following types:
- Inguinal hernia: The intestine or bladder passes through the abdominal wall into the groin. Inguinal hernia is the most common type of hernia, especially among men due to a physical weakness they have in this area.
- Femoral hernia: It occurs when the bowel enters the canal that carries the femoral artery to the upper thigh. Hernias are more common in women, especially those who are pregnant or obese.
- Umbilical hernia: A portion of the small intestine passes through the abdominal wall near the navel. Common in newborns, it often affects obese women or those who have had multiple labors.
- Epigastric hernia (Abdominal hernia): It appears in the midline of the abdomen, usually above the navel.
- Postoperative abdominal hernia: The bowel passes through the abdominal wall at the point of an incision from previous surgery. This type is more common in the elderly or overweight individuals who are inactive after abdominal surgery.
- Sports hernia (Link): Sports hernia (or athletic pubalgia) is one of the posterior wall (floor) abnormalities that cause pain in the groin. This condition is caused by the gradual weakening of the posterior wall of the inguinal canal, resulting in a hidden, indirect inguinal hernia.
- Rare types (Spiegel, Richter, Littré’s hernia, lumbar hernia, obturator hernia, sciatic hernia, etc.)
How is a Hernia diagnosed?
The diagnosis begins with a detail patient history and physical examination by the doctor.
A series of imaging tests may then be necessary, such as:
- Abdominal ultrasound
- Computed tomography (CT)
- Magnetic resonance imaging (MRI)

How are Hernias treated?
Hernia repair is carried out exclusively with surgery. In general, hernia repair involves closing the opening in the abdominal wall. This is usually achieved using a surgical mesh.
There are different surgical methods for repairing each type of hernia, such as conventional open surgery, which involves making a large incision, or minimally invasive techniques, such as laparoscopic and robotic repair, which are performed through very small holes in the abdomen and cause the least possible injury of neighboring tissue.
In recent years, minimally invasive techniques are preferred over open surgery, as they are accompanied by significant advantages.
Laparoscopic Hernia Repair
What is Laparoscopic Hernia Repair?
Laparoscopic surgery allows a hernia to be repaired in a minimally invasive way, ensuring the least possible injury to muscles and other tissues of the abdomen, which is especially important for professional athletes.
The laparoscopic method involves not incisions, but the opening of small holes through which the surgical instruments are inserted, including the laparoscope. The latter includes a special micro-camera that allows the surgeon to view the hernia and the surrounding tissue in magnification on a screen.
Repair also involves placing a mesh at the location of the hernia.
How is Inguinal Hernia repaired laparoscopically?
The operation is performed through 3 holes:
- one hole 8 mm wide, below the navel, from where the high-definition optical laparoscope is inserted, and
- two holes 5mm wide, in the midline, low in the abdomen, through which the other instruments are inserted
The laparoscope is connected to a high-definition screen. With a microsurgical technique, the hernia is corrected, and the weak abdominal wall is strengthened with the placement of a mesh. The mesh, measuring 10 × 15cm, is non-absorbable and perfectly compatible with the human body.
Dr. Konstantinidis and his Surgical Team employ the extraperitoneal technique (TEP – Totally Extraperitoneal Repair) (Link), which is regarded as the safest method of inguinal hernia repair with the least possible complications.
This technique has been applied in our clinic since 1991 with a recurrence rate of less than 0.5%.
Dr. Konstantinidis and his Surgical Team have a total experience of more than 3,000 inguinal hernia repair surgeries, considered to be one of the most extensive in the world.
What is a Laparoscope?
The laparoscope is a long and thin a fiber-optic instrument that allows surgeons to project and view the part of the abdomen (“lapara” in ancient Greek) that interests them. The laparoscope is connected to a video camera and a cold light source that allows the surgeon to view the image on a TV screen.
This technology allows surgeons to operate through small incisions (of a few millimeters) and achieve an excellent view of the organs and structures involved in the operation.
What are the advantages of Laparoscopic Hernia Repair?
A great advantage of the TEP laparoscopic method is that it is performed extraperitoneally. This means that the surgeon does not open the abdomen. Instead, he creates a “pocket” between the peritoneum and the muscles, at the point of the hernia, and places the mesh there, to achieve the desired stability and to repair the original problem. In this way, the least possible injury from the operation is ensured.
A second advantage is that with laparoscopy the surgeon’s access to the problem area is much better and this allows the placement of larger meshes, e.g. measuring 10 X 15 cm or more, covering a large part of the inguinal area.
Thus, the chances of a relapse are dramatically reduced.
This option is not offered in open surgery, as the surgeon’s access is more limited.
What preparation is required before surgery?
- It is best to avoid eating and drinking liquids after midnight the night before.
- Take a bath the day before or the morning of the operation.
- Your surgeon may decide to give you a laxative the day before or have an enema.
Depending on your age, choice of anesthesia and concomitant conditions, tests such as:
- General and blood coagulation test
- Electrocardiogram and cardiological examination
- Chest X-ray
Most hernia repair surgeries require one day of hospital stay.
Often the patient can be discharged the same day. In this case, you arrive at the hospital on the day of the operation and are discharged the same day.
Do not shave the area near the hernia before surgery (it could increase the rate of infections). If needed the surgical team will do this as soon as you are transported to the operating room.
Medications such as aspirin, anti-inflammatory drugs, anticoagulants, and some arthritis medications may need to be stopped 7-10 days before surgery.
Give all the information about the medicines you are taking to your doctor in time.
Is it likely for laparoscopic surgery to turn into an open one?
No, it is rather unlikely. In some patients, however, for special reasons, the operation may need to be converted to open surgery.
Conversion to the conventional open technique is sometimes necessary for technical reasons and is not considered a complication of the operation.
What to expect after laparoscopic hernia surgery?
- You will be discharged from the hospital when you can drink some fluids, urinate and be able to rise and walk.
- You can return to most of your activities in a few days.
Although you will feel well immediately after surgery, we usually urge patients to rest for a few days.
- It usually takes patients 1-2 weeks to fully recover.
- No matter how well you feel, your surgeon should see you again one week after surgery.
How can I reduce the risk of my Hernia recurring?
We recommend that you avoid weightlifting or any other strain on the area (e.g. strenuous exercise with increased intra-abdominal pressure) immediately after your operation. Make sure you let us know before you return to this type of activity.
Other precautions include:
- Avoid severe constipation (high fiber diet)
- Elimination of chronic cough (smoking cessation)
- Elimination of dysuric symptoms (prostate monitoring in men)
- Proper exercise that does not strain the lower abdominal muscles
What is the TEP method?
Completely extraperitoneal endoscopic hernia repair with mesh placement (Totally Extraperitoneal – TEP), is the most modern laparoscopic method and offers better results.
Hernia repair is performed through 3 holes 5 mm long in the skin, without cutting the muscles.
The advantage becomes even more obvious when the hernia is bilateral, so the correction can be made through the same holes, without the need for a new incision.
The surgeon works with a special camera and with a magnification of 10-15 times, while the operation is completed quickly, without blood loss and with great precision.
Robotic Hernia Repair
What is Robotic Hernia Repair?
Robotic surgery is the evolution of laparoscopy and offers significant advantages over the latter, ensuring the best possible access to the problem area and unsurpassed accuracy and flexibility in the surgeon’s movements.
Thus, the best possible medical result is achieved, even for the largest and most difficult hernias.
There are various robotic hernia repair techniques applied by Dr. Konstantinidis and his Surgical Team with great success, depending on the type of the problem:
- The TAPP (Transabdominal Pre-peritoneal) method is intraperitoneal and is performed with the help of a robotic system. As a technique, it offers a significant advantage, especially when it comes to repairing large and complex hernias. During TAPP, the surgeon enters the peritoneal cavity and places a mesh through a small peritoneal incision at the site of the hernia.
- TARUP (Transabdominal Retromuscular Umbilical Prosthetic) is a robotic laparoscopic technique, in which the surgeon creates a “pocket”, as in the laparoscopic TEP method, which also includes the fascia of the rectus abdominis. In this way, the “pocket” becomes stronger, allowing larger meshes to be placed. The extension of the “pocket” to the side is called TAR and includes the incision of the fibers of the transverse abdominal muscle to close the hernia gap more easily without tension.
- The IPOM (Intraperitoneal Onlay Mesh) method is a special hernia repair procedure, in which a mesh is inserted into the abdominal cavity and placed from the inside. In this method, double-sided meshes are placed: one side is rough and faces the abdominal wall. On this rough surface, natural tissue develops that gradually integrates into the body. The other side of the mesh is a smooth surface, which contains a substance that prevents the intestines from adhering to it. When the hernia opening is closed with sutures before the mesh placement then the method is called IPOM plus.
- New methods of robotic extraperitoneal repair that are summarized under the general term E-TEP have already started to be applied in our clinic and in selected cases with excellent results.
What are the advantages of Robotic Hernia Repair?
Robotic hernia repair has many advantages, such as:
- Minimal tissue injury, since the large incision of the open surgery is avoided
- Minimun blood loss
- Less postoperative pain
- Avoidance of complications and minimal risk of recurrence
- Faster recovery and return to daily activities and sports
In addition, the robotic hernia repair techniques applied by Dr. Konstantinidis and his Surgical Team offer significant advantages for the treatment of large hernias, with a diameter of more than 7-8 cm.
In the case of large or complex hernias, the use of the robotic system does make a difference, with its particularly fine tools, as it ensures:
- Unsurpassed surgical precision
- Great ease of movement and flexibility
- Optimal access to the affected area
Thus, the repair of large and difficult hernias is minimally invasive and open surgery is avoided.
What happens after Robotic Hernia Repair?
Recovery after surgery is immediate. The patient is mobilized from day one and is usually discharged the same day. However, if the hernia is large and the patient needs follow-up, then up to 48 hours of hospitalization may be required.
The return to daily activities is again immediate and the patient is fully functional from day one.
The return to sports activities takes place within 4-6 weeks after the operation, a period of time significantly shorter compared to the 3-4 months of avoiding similar stress, required after open surgery.